Dr. Max Ezzati: Basically, women are born with a limited nonrenewable endowment of eggs at the time of birth. This is a very precious thing that is not going to be replaced during the following years of life. As a matter of fact, women are born with about 1,000,000 or 2,000,000 eggs at the time of birth, but then that number already drops about 400,000 at the time of puberty and the beginning of menses, so we lose about 1.6 million eggs from birth until starting periods.
That number is pretty much determined genetically at the beginning, but the catch is that not everybody is born with the same number of eggs and not everybody is losing the eggs at the same pace. At any given period in life, women may have a different number of eggs and different residual balance in their egg bank account.
Dr. Aimee: Are there some misconceptions that people often have about the number of follicles that they have in their ovaries?
Dr. Max Ezzati: Basically, it’s very difficult to know the exact number of follicles left in a woman’s ovaries, because the only way to know that for sure is to take out the ovaries, slice them into pieces, and look at it under the microscope, which is not what we do of course. We have to rely on some surrogate markers that can give us some estimate of the number of follicles left in a woman’s ovary.
That brings us to ovarian reserve testing, which would be in the form of a series of blood tests and ultrasound. By doing the ovarian reserve testing, we get some estimate of the number of follicles in the ovary, but we don’t necessarily get the whole picture. The other issue is that there is some significant variability in these test results from one month to the next within the same individual. That’s why we don’t rely on one single test to get a good understanding of a woman’s ovarian reserve.
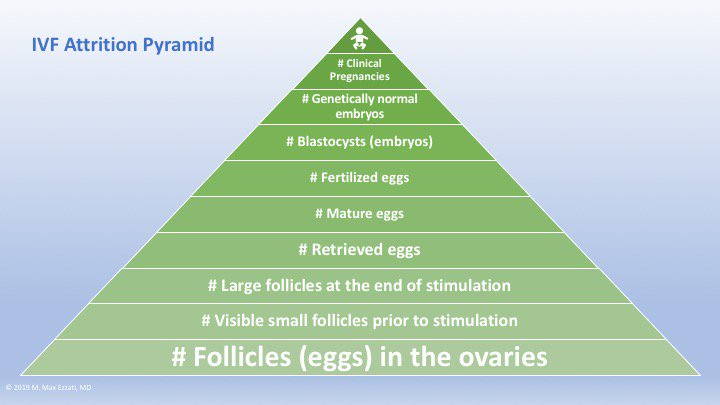
Dr. Aimee: Right. The next layer in the pyramid is the visible small follicles prior to stimulation. What is a follicle and what determines how many you see?
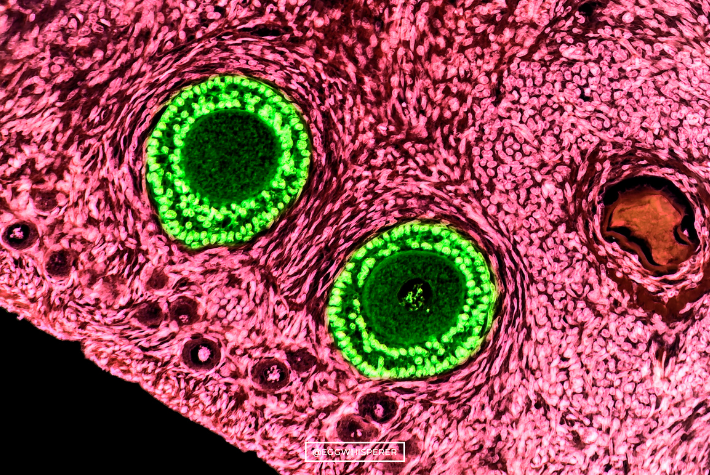
Dr. Max Ezzati: Because eggs are very precious and they are not going to be replaced, the body is going to take care of the eggs by placing each and every single one of them in a safe box that I call a follicle. I basically call a follicle a safe box that is protecting the egg inside of it. There is a one-to-one relationship between the eggs and the follicles. During fertility consultations, these names, eggs and follicles, are used interchangeably. Most of the time they are referring to the same concept, but they are not exactly the same thing.
The fact that they are not exactly the same will have an impact on the fertility pyramid, because what we can see on ultrasound is just the follicle, we don’t see the eggs inside of the follicles. The number of follicles that we see doesn’t necessarily mean that we are going to have an equal number of eggs.
Generally speaking, every month, I use another analogy, I say several hundred follicles wake up and register at the school of egg development. These eggs register at the first grade, some of the first graders make it to the second grade, but some drop out. Some of the second graders make it to the third grade, but the rest drop out. As they grow in size, but they drop in number, once they reach middle school, they become large enough to be seen on ultrasound. The follicles that we see on ultrasound at the beginning of the cycle are the kids that have already made it to the middle school.
I can do an ultrasound, get an assessment of their number. If there is no fertility treatment, only one of those follicles in middle school will keep growing to become the one that graduates that month, but with the help of the medication that I call the private tutoring that come on board to help the middle schoolers, we basically make sure that extra follicles that were going to be drop outs are not going to drop out and are going to go all the way to graduation.
Dr. Aimee: I love it. Is there anything else aside from private tutors that we can do for them not to drop out or to do better. To see more eggs is basically what I’m asking. Is there anything that a woman can do to increase the number of follicles that you see? I get that question so much and I’m sure you do as well.
Dr. Max Ezzati: Absolutely. I always say that the number of kids that graduate from high school depends on two things. Number one, how many kids do we have to work with equals the number of eggs that we have to work with. Also, what is the quality of the teacher and the curriculum that comes on board and works with those kids.
If we are not graduating, in other words if we are not getting enough eggs at the end of the stimulation, it could be because of two reasons. Either we don’t have enough eggs to work with, unfortunately that’s a very difficult situation to deal with, or maybe it’s because we do have eggs, but the curriculum and the teachers were not doing the job that they were supposed to do.
So, we do have influence over the modifiable factor of teachers or the stimulation protocol that we can look into and figure out if that stimulation works best for those number of eggs or not, and then modify and tweak it for the next cycle if it did not get enough eggs. But if the underlying problem is the low number of eggs, that is a very difficult thing to do.
However, some studies have shown that some supplements, for example, mild forms of androgens like DHEA supplementations, can potentially help some of the, I will call them second or third graders, to graduate into the fifth or sixth grade, to middle school, and therefore when the private tutor comes on board, they may have a few more follicles to work with. Some people have advocated for supplemental DHEA as a way to get a few extra follicles at the beginning of the stimulation to work with, but it doesn’t work in everybody.
Dr. Aimee: Right. I wish there was some sort of pharmacogenetic testing that we could do at the beginning to see who could potentially benefit from some of these supplements. One day.
The next layer up in our fabulous pyramid that you have invented is the number of large follicles at the end of stimulation. Not to make a joke, but why does size matter?

Dr. Max Ezzati: The size matters because the quality or the maturity of the egg within the follicle depends on the size of the follicle. In other words, if the egg inside the follicle is going to be mature and usable for the purpose of fertility and ultimately resulting in the formation of a competent embryo, that egg needs to have had enough training and enough education within that follicle. Follicles that are very small usually do not have a mature egg inside of them. Follicles that are on the larger side usually have a mature egg inside of them.
However, again, it is also important to know that size is one of several factors that determines what is the quality of the egg inside of them. In other words, sometimes we can even have a big follicle that does not have a mature egg in it, and sometimes we may get pleasantly surprised and have a fairly small follicle that has a mature egg in it. It’s not a 100% black and white situation. It’s one of the several factors that help us determine how many eggs we are anticipating to retrieve.
Dr. Aimee: Why do some follicles reach larger sizes and some don’t?
Dr. Max Ezzati: It probably depends on how responsive the cells that build the walls of the follicles are to the private tutoring or to the stimulation, because some of those cell walls are more likely to respond and grow faster, some of the follicles are less likely to respond.
Again, going back to the egg development school analogy, we know that regardless of how good the teachers are, unfortunately, some kids do not have the same capacity as others. Teachers come on board, but not all of the students are going to respond equivalently and to the same level, so it also goes back to the potential of the eggs for growth on their own.
Dr. Aimee: Okay. Let’s go back to your IVF Pyramid. The next layer up is number of eggs retrieved. What affects your egg count at egg retrieval and how do you know when it’s time for retrieval? Does the estrogen help you at all during this process?
Dr. Max Ezzati: We usually make that determination based on two different factors. One, by imaging and ultrasound based on the size of the follicles, as we discussed. The second one based on blood tests and the estradiol level, which is a functional measure of the follicles’ capacity.
Estradiol is a hormone that is being secreted and synthesized by the cells that are making the walls of those follicles containing the egg. So, if follicles are still responding and are still growing and are functional, they secrete estradiol or estrogen. We rely on that estrogen level as a surrogate marker for the function of the follicles.
Dr. Aimee: Okay, now we’re going up to the next layer. That is the number of mature eggs. Why does egg maturity matter and what causes the eggs to actually mature?
Dr. Max Ezzati: When it comes to maturity of the eggs, we have to try to differentiate between two different types of maturity of the eggs. Most of the time when we are using these words, we are referring to the nuclear maturity of the eggs, meaning that the egg has completed the process of receiving only half of the chromosomes from the female.
As human beings, we have 46 chromosomes, we get 23 chromosomes from dad in the sperm and 23 chromosomes from mom from the egg. In order for the egg or sperm to have the correct number of chromosomes, the initial 46 chromosomes in the progenitor cells need to divide equally and symmetrically into two 23s, half each.
When we are talking about nuclear maturity of the egg, we are talking about the eggs that have completed the process being ready to have only 23 chromosomes. This is important because when we are pushing the eggs towards maturation, towards graduation, with the private tutoring, some of the kids may make it to maturation to graduation but may not be quite ready yet because they were pushed a little bit too excessively. Because of this, there is always a fraction of the eggs that we retrieve that are truly ready to be fertilized.
There is another aspect of maturity, which is called cytoplasmic maturity, but that is not an aspect that is easily identifiable or can be checked during the process. We just hope that during the course of the stimulation the eggs within the follicles have had enough time to achieve both nuclear and cytoplasmic maturity.
For example, if the stimulation has been very short, we think maybe the cytoplasmic maturity has been impacted. On the other hand, when the stimulation is getting too long, we get concerned about the cytoplasmic competence of the eggs.
Dr. Aimee: If an egg isn’t mature at the time of egg retrieval, is there anything the IVF lab can do reliably to help it mature?
Dr. Max Ezzati: It depends how immature it is. In other words, it depends how far from being ready it is. If it is what we call metaphase one, so just one step behind being ready, then occasionally that egg can mature within the few hours that the eggs are being incubated in the lab and potentially can be used for fertilization. In rare instances, the eggs can mature overnight and can potentially be used for fertilization the next day. But generally speaking, these are not common scenarios. We expect the eggs to be mature at the time of the retrieval.
Dr. Aimee: You talked a little bit about eggs potentially being too mature. Is there ever such a thing as having an overcooked egg?
Dr. Max Ezzati: I believe there is. There is no good way to recognize that, but most studies have shown that if follicles get too big, based on their size, we’re talking about 24 or 25 millimeters, for example, that’s really too big. Most of the time, we expect or we think the eggs may get overcooked, and that’s a time that we try to avoid. We try to get to the eggs before they get overcooked.
Dr. Aimee: Aside from maturity, is there anything else you can tell about the egg, like the quality?
Dr. Max Ezzati: When embryologists look at the egg, they usually describe the egg in morphological or appearance terms. They say whether the eggs had a dark appearance or a more uniform appearance, they talk about the contours or the periphery of the cells. But it’s important to know that these appearance-based assessments are very subjective and are not necessarily correlating with the eventual outcome of the embryo that will result from that egg.
Really, maturity of the egg currently is mainly assessed in an objective way by visualization of what we call a polar body to see whether the egg is ready to fertilize, whether it has completed that process of separating the chromosomes symmetrically. Other than that, embryologists usually comment on the quality of the eggs, but this doesn’t necessarily correlate with the actual outcome, which is the developmental potential of that egg.
I always say never judge a book by its cover. The egg may look good, but may not actually have what it takes to become a good embryo. Otherwise, the egg may not necessarily look very good, but it may result in a beautiful embryo that results in a beautiful baby.
Dr. Aimee: I agree. The next layer up on our pyramid is the number of fertilized eggs. How do you fertilize eggs in the lab?
Dr. Max Ezzati: Generally speaking, there are two ways to fertilize the eggs.
The conventional method to fertilize the egg is called conventional insemination, which means that we put each and every egg, without cleaning them first, next to about 50,000 to 100,000 sperm, and then we sit back and cheer for the fetus sperm to fertilize the egg. In other words, we don’t do anything. One of those sperm is going to make it into the egg on its own, this is survival of the fittest. This is the conventional or the standard IVF.
However, the problem that not all men have enough sperm to enable the sperm to make it into the egg on its own. In situations where sperm motility or count, or even the appearance and morphology of the sperm, are on the lower side, then we have a procedure called ICSI, which stands for intracytoplasmic sperm injections, in which the embryologist picks up just one single sperm, puts that into a needle, and then injects a single sperm under the microscope into the egg.
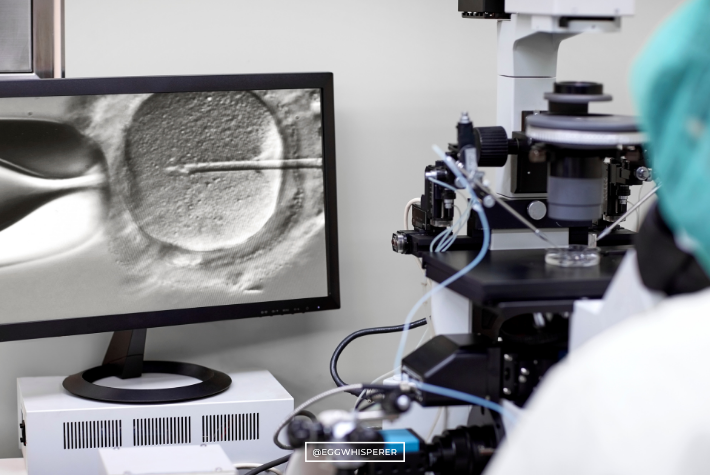
ICSI is another alternative way of fertilizing the egg. It’s usually used for couples in whom the male partner does not have good quality sperm and has some major issues going on with semen parameters. Since its introduction in 1991 and 1992, it has revolutionized the treatment of male fertility.
However, because it results in a slightly higher fertilization rate, about 60–70%, some centers and some couples decide to do ICSI as a default method of fertilization for everybody. In principle, there is nothing wrong with this approach, but this is a hotly debated topic, whether you are going to recommend ICSI for couples without male factor or not. That is a separate topic, basically.
Dr. Aimee: Can ICSI cause birth defects or damage to the egg?
Dr. Max Ezzati: ICSI is operator dependent, which means that the outcome of the ICSI depends on the experience and the training of the embryologist or the scientist who is actually doing the procedure. It’s also very important to know that even the best and highly skilled embryologist every now and then may not have a good day. The fact that ICSI sometimes does not work can potentially, in some instances, be explained by operator issues.
However, it’s not the only potential drawback with ICSI. The other issue with ICSI is that we don’t really know which sperm we are choosing to inject. The selection of the sperm is also a little bit subjective. Both the subjective nature of the sperm selection as well as the issues with the operator can potentially result in problems with ICSI. Specifically, about genetic problems.
There are a series of medical disorders that are actually called epigenetic disorders that are not per se problems specifically with changing genetic code, but a problem with the way the genes are expressed. These medical epigenetic conditions are very rare. In the general population, they may happen 1 out of 10,000 or 1 out of 15,000 cases.
Some studies have shown that if the eggs have been fertilized via ICSI, the resulting children from these embryos can potentially have a slightly higher relative risk of having epigenetic disorders. How much higher? Let’s say from 1 in 10,000 it might increase to 1 in 1,000 or 1 in 500.
So, the relative risk may be increased, but the absolute risk remains very low. I would say 99.9% ICSI does not result in birth defects. But if you want to compare ICSI with conventional, then conventional is probably just a tad safer.
Dr. Aimee: Got it. Going back to eggs and fertilization, how do you know if an egg is fertilized?
Dr. Max Ezzati: Embryologists have a fairly narrow window of time, about 18 hours after the eggs have been exposed to a sperm either via ICSI or via conventional insemination, to check for fertilization. They usually call it a fert-check. That is done in the morning, usually at 8:00 AM to 10:00 AM, because of the fairly narrow window of time.
When embryologists look at the eggs that have been previously exposed to a sperm, again either via the conventional way or via ICSI, they are expecting to see two polar bodies and two per nuclear, which are referring to remnants of those chromosomal compartments that are currently being shaped to form a mature embryo. If an embryologist looks at the eggs and sees these structures, they will declare the egg as fertilized.
Again, it is important to know this is a time-sensitive issue, so occasionally the embryologist may not be able to call the egg fertilized correctly on that day, but then a few days later they will see the egg and now the embryo has been growing appropriately, so they may occasionally change their original assessment and say, “At the time I did not see the evidence of fertilization, but a few days later we see evidence of growth indicating that the egg had fertilized correctly. We just did not check it right at the correct time, that’s why we missed the window.”
Dr. Aimee: Got it. That’s probably maybe a zero PN, it’s called zero, but it just means they missed the window.
Dr. Max Ezzati: Absolutely. We see that fairly often, actually, every now and then, that zero PN or even 1 PN may continue cleaving and resulting in a very good quality embryo, and then we’ve had babies from those embryos.
Dr. Aimee: Yes. Going back to our pyramid, we’re making our way to the top. The next layer up is the number of blastocysts. What is a blastocyst?
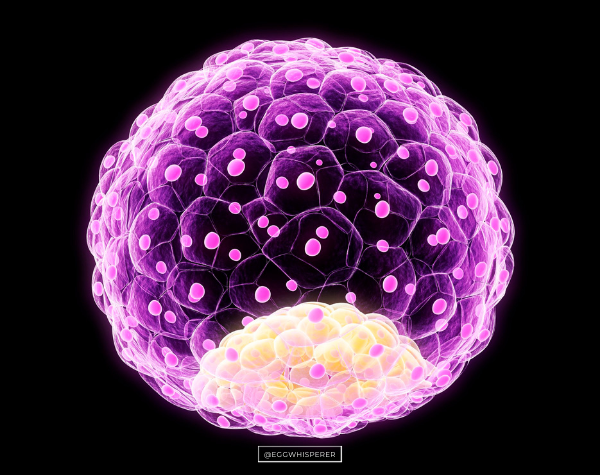
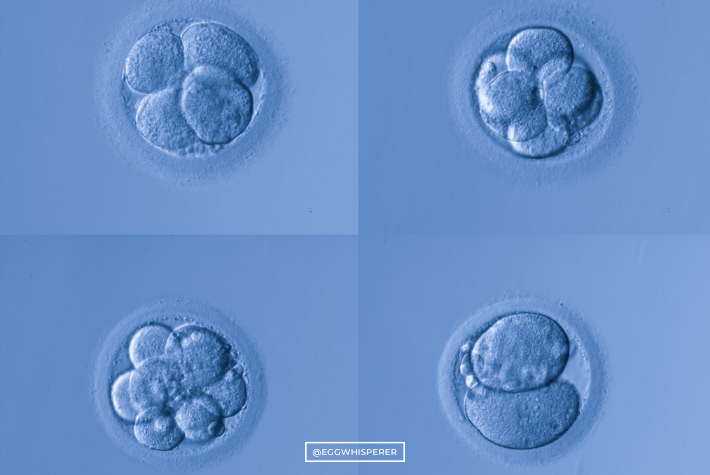
Dr. Max Ezzati: A blastocyst is an embryo. Once the egg gets fertilized via the sperm and forms a one-cell embryo, then in the next few days it is going to divide successively. After two days, it usually has about four cells. Then it divides into eight cells on day three. On day four, somewhere around 16 cells. Then around fay five and six, it usually ends up having somewhere between 100 to 200 cells, and also changes its shape into a very distinct structure called a blastocyst.
In brief, a blastocyst is a more advanced embryo, is a more advanced stage that is reached after five to six days of continued appropriate embryonic growth.
Dr. Aimee: Why do some embryos stop growing before they reach that stage?
Dr. Max Ezzati: That’s a very good question. It could be because of a variety of reasons. It could be because of the problems with the egg quality, or it could be problems with the sperm quality. We don’t really know most of the time what was the initial culprit. Occasionally, but not commonly, it can also be because of the incubator conditions in the lab.
Maybe, for example, if this embryo was placed in the uterus at an early, maybe it would have made it into a blastocyst, but because we kept it outside it did not go all the way. Whether there are some inherent issues with the egg or sperm that have formed the embryo or whether there were problems with the embryology lab and the culture condition, it’s not always easy to say and to make that distinction.
Dr. Aimee: Does the quality of the blastocyst matter?
Dr. Max Ezzati: Absolutely. That is one of the major factors that is going to determine whether this blastocyst once transferred into the uterus is going to result in the formation of an ongoing pregnancy and eventually a healthy baby.
There are different ways for us to assess the quality of the blastocyst. The easiest way or the traditional way is by looking at it under the microscope and then counting the number of cells that the blastocyst has. Again, we will not be able to count each one of them individually, but we get some idea. We look at their shape, look at their symmetry, look at the cavity or the hole that is expected to appear within the blastocyst. We call this morphological or shape-based assessment of the blastocyst.
We usually give them a grade. This is the standard way. We can even do a more thorough assessment of the quality of the blastocyst, particularly at the genetic level, by doing preimplantation genetic testing, which entails removing a few cells from the embryo and then biopsy them to see if the embryo has the correct number of chromosomes or not.

Dr. Aimee: Perfect. That’s the next layer, the number of genetically normal embryos. What does genetically normal actually mean? You mentioned a little bit already about how it’s determined. Can you talk a little bit more about that?
Dr. Max Ezzati: Genetically normal is referring to the number of chromosomes that the embryo has. By that we mean the embryo that has 46 chromosomes and only 46 chromosomes, no more chromosomes, no fewer chromosomes.
The body does not tolerate any extra or any missing genetic information. It needs to have the exact number of chromosomes. In order for the embryo to have the correct number of chromosomes, it needs to get the correct number of chromosomes from its ingredients, which are the sperm and the egg.
Again, if the egg is of good quality, we usually expect the embryo resulting from that egg to be of good quality. But I do not want to ignore the sperm, because the sperm also plays a significant role, basically half of the chromosomes do come from the sperm. It’s not always easy to say whether an abnormal number of chromosomes were due to problems with the egg or due to problems with the sperm.
Dr. Aimee: What can people do to increase their chances of having a genetically normal embryo?
Dr. Max Ezzati: Having babies earlier. That’s really the most important factor that can determine that. Generally speaking, in order to have a genetically normal embryo, we need to have genetically normal eggs and genetically normal sperm.
On the sperm side, it’s very important for the men who are planning to have a baby to have healthy diets full of antioxidants to improve the quality of the sperm DNA. It’s important for them to have frequent ejaculation, to have fresh sperm available for the day of the egg retrieval.
On the female side, again good diet and healthy diet is definitely important. Exercise, reducing weight. These are the things that can potentially have a positive impact on the egg quality. But the most important factor on the female side is the age, which is unfortunately not a modifiable factor.

Dr. Aimee: Right. I wish. The next layer up is the number of clinical pregnancies. This is the thing. If an embryo has normal genetics and is good quality, why wouldn’t it turn into a pregnancy?
Dr. Max Ezzati: That is a very good question. I get that question all the time, as I’m sure you get asked that all the time. When we transfer a reportedly normal embryo into the uterus that looked good on ultrasound and we had the perfect transfer, why didn’t it work?
If an embryo transfer is not successful, I usually break it down into two components. Either the embryo was not good or the uterus was not good. Most of the time, if an embryo transfer is not successful, we usually blame the embryo 80–90% of the time. About 10–20% of the time, the transfer is not successful not because the embryo was not good, but maybe the uterus was not optimally prepared or ready to receive the incoming embryo.
On the embryo side, it’s important to know that even a reportedly normal embryo is not guaranteed to be normal, because there could still be a variety of genetic issues that are present in the embryo but unfortunately were not detected by the genetic testing that we had done on the embryo. This is due to a variety of reasons, because of the biological limitations that the cells that we sample are not necessarily the cells that matter, because of a process called mosaicism.
Also, because of some technical issues with the fact that we have to work with only four, five, or six cells, and then we have to amplify the DNA of these very few cells. Sometimes there can be problems with the amplification. In other words, in order to make the DNA readable, sometimes not all parts of the DNA are basically readable to the same level and to be the same clarity.
Also, the resolution of the test is not 100% accurate. I always give the example of some textbooks, saying that with the genetic testing we are going to look at the genomic library of the embryo and then make sure that there are 23 textbooks on the maternal side and there are 23 textbooks on the paternal side, for a total of 46 books, or chromosomes.
We also have the ability to pick up a textbook, look at it, glance at it, making sure it has all of the chapters. Occasionally, we may even check some of the pages. But we don’t have the ability to go and read each paragraph, each sentence, each word, and each letter. Sometimes a missing paragraph is enough to cause the embryo to be nonviable, but that was not necessarily picked up by the test.
Dr. Aimee: Why not? You would think that at this point in time we would be there, that we could pick everything up. But it’s so incredibly frustrating. I imagine you feel the same way.
Dr. Max Ezzati: Absolutely. It’s really frustrating when couples have been through so much in the IVF process and they have eventually made it to the point of having a reportedly euploid or normal embryo, and now their hopes and our hopes are very high that this is the one, this is the embryo that is going to result in the delivery of that healthy baby that we are all hoping for, but then we transfer and it does not result in a pregnancy. It’s very heartbreaking.
Dr. Aimee: It is. Also, experiencing a miscarriage after you go through all of that. What are the chances of a miscarriage after transferring a genetically normal embryo that is high quality?
Dr. Max Ezzati: Usually, this number is reported to be somewhere between 8–12% of the time. It’s still a high number. I still would like that to be really much lower than that, like to zero. At least, the good thing is that number is independent of the female age, which means that if the embryo is reported as normal across all age brackets, whether that woman is 32 or whether she is 42, we are going to have somewhere about 8–12% maximum of miscarriage rate.
Dr. Aimee: I had to look this up before coming on with you today, what the peak or apex of the pyramid is called. Apparently, it’s called a pyramidion. Did you know that?
Dr. Max Ezzati: I did not know that.

Dr. Aimee: Now we’re there. The pyramidion is a live birth. I feel like we need to start singing a song or creating a new song, Talk Like an Egyptian, now let’s start pyramiding. We have to create song lyrics to get people to understand everything there is to understand about your IVF Pyramid. I want to basically start pyramiding right now. That’s going to be a thing, let’s pyramid together.
Can you describe what an IVF pyramid would look like? I’m going to give you a whole bunch of scenarios, so bear with me. Let’s start with a 25-year-old with 10 follicles. What would her pyramid look like?
Dr. Max Ezzati: A 25-year-old with 10 follicles, I’m assuming at the beginning of the stimulation, 10 small follicles, it’s important to know from the very beginning we are dealing with a little bit of a low number of follicles for a 25-year-old. In that age bracket, we are usually expecting about 15 or 20 follicles. But the good thing about this particularly young lady is that her egg qualities are expected to be very good, so the low number to begin with at the beginning is not as major of a concern as it would have been in an older woman.
Let’s say out of the 10 I’m expecting to have about maybe 8 or 9 at the end of the stimulation for the large follicles. Out of those 8 or 9 large follicles, hopefully, we get about 7 or 8 eggs. Hopefully, about 6 or 7 of them are mature. Then when we try to fertilize them, hopefully about 4 or 5 will fertilize. Out of the 5 fertilized, our blastocyst conversion rate is somewhere around 50–55%, a little bit higher for younger women, so if we are lucky, we may get 3 or even 4 blastocysts. If we are unlucky, 1 or 2.
Let’s say 3 blastocysts from a 25-year-old. The chances of them being genetically normal for each one of them is about 55–65%, so hopefully one of those or maybe two of them normal. Then when we transfer the normal embryo, the chance of that resulting in a pregnancy is about 65%. Then about 10% risk of miscarriage. About 55% actually having a baby.
Dr. Aimee: I love it. There should be IVFpyramid.com where you just plug in your numbers and your numbers come up. It would be a great counseling tool.
Let’s go now to a 35-year-old with 10 follicles.
Dr. Max Ezzati: This is a more appropriate number of small follicles to begin with for a 35-year-old. Out of 10, we are expecting to get the same number of large follicles and the same number of mature eggs, so somewhere around 8 or 9 large follicles and 7 or 8 retrieved eggs, then 6 or 7 mature eggs. Then when we try to fertilize them, about 5 fertilized eggs.
Here, we may expect a little bit fewer blastocysts. Not that much different compared to a 25-year-old, because 35 is still pretty young. We may get let’s say 2 blastocysts out of the 4 to 5 fertilized eggs. At age 35, probably about 50% of those embryos are euploid or normal, so hopefully one of them is going to be normal. If we transfer that embryo, she has about 65% chance of pregnancy and 55% chance of going all the way to term.
Dr. Aimee: Okay. The next one is 40-years-old with 10 follicles. What would her IVF pyramid look like?
Dr. Max Ezzati: We are approaching difficult terrain. With a 40-year-old, out of the 10, we may get about 7 or 8 of them making it to the large follicles. When we try to retrieve the eggs, we probably get maybe 5 or 6 eggs. Out of the 5 or 6 eggs, let’s say 4 or 5 of them are mature. When we try to fertilize them, maybe 3 or 4 fertilize.
Then out of these 3 or 4, we may get 1 or 2 blastocysts. Then the chance of each blastocyst being chromosomally normal at the age of 40 is only about 30–35% at most. Hopefully, she will have a normal one among them, but the chances are that she needs to have 3 or 4 blastocysts at that age to have one normal one.
Dr. Aimee: Right. Okay, last pyramid for us to go through. 45-years-old and 10 follicles.
Dr. Max Ezzati: A 45-year-old with 10 follicles, we are probably going to have maybe 6 or 7 at most with the large follicles at the end of the stimulation. When we try to retrieve eggs, probably we may get 5 eggs. Out of the 5 eggs, probably 4 are mature. When we try to fertilize, maybe 2 or 3 fertilize.
Then if we wait for five days to see if they make it into a blastocyst, we may have one, or we may have none out of the 2 or 3 fertilized eggs. If we are lucky to have one, the chances of that being normal at age 45 is only about 10% or less. She has a chance, but the chance is about 10%.
Dr. Aimee: Right. I appreciate you going through all of the levels of the IVF pyramid. I think the one thing that people listening will notice is that the number 10 doesn’t increase to 20. I think that’s a huge misconception. Like you said at the beginning of our interview, that people somehow have this misunderstanding as to what happens as you go along the way, and one thing people think is we have the power to turn 10 eggs into 20. We certainly don’t. MD stands for medical doctor, not deity or superpower.
Dr. Max Ezzati: I agree. Unfortunately, that’s a very important concept to clarify at the beginning of the fertility journey, just to say that there are limits to what we can do as fertility doctors and there are limits to what medicine can do in this specific situation. At least, for the foreseeable future. Maybe at some point we’ll be able to create novel new eggs. I think at some point it will happen. I don’t think it’s going to happen next year, but maybe in 5, 10, or 15 years we’ll have that ability. Until then, we are dealing with a very precious commodity called eggs.
Dr. Aimee: Thank you for creating the IVF Pyramid. It has helped people all over the world. I talk to everyone about it in my IVF class. I’m sure that your patients appreciate you so much for what you do. Thank you.
Dr. Max Ezzati: Thank you very much for having me. It was great to be with you. I’m glad you’ve found it helpful.
Catch more of me and topics like this through The Egg Whisperer Show. Episodes are live-streamed on YouTube, Facebook, Twitter, IGTV and Apple Podcasts . Sign up to get my newsletter. Tune in to The Egg Whisperer Show on YouTube. And sign up for The Egg Whisperer School.


