It seems like everyone is doing IVF. You hear about it in the news. You hear about it in different articles. You hear about it from your neighbors, your friends, so many different people are doing IVF. Everyone is giving different bits of information, but what are you supposed to believe?
Today I want to share about the risks of IVF so you know what you’re getting yourself into.
What is IVF?
I think one of the first important things to do when thinking about IVF is to know what IVF is. I jokingly say, and a patient of mine taught me this, that IVF stands for “Is Very Fun.” I mean, I try to make IVF as fun as possible, but at the end of the day, it isn’t.
IVF involves taking an egg and putting it with the sperm, and then they kind of do a little bit of this and a little bit of that, with maybe some Barry Manilow playing in the background. The result is an embryo. This is what an embryo looks like:
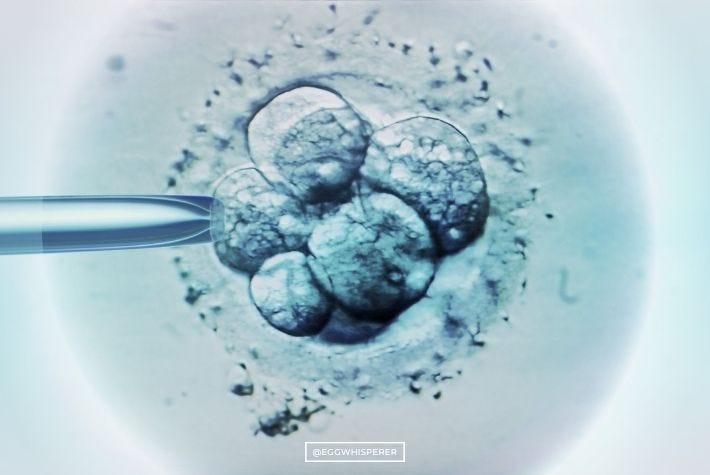
As you’re going through the process with me, I’ll talk to you about what your embryos are doing. I’ll give you updates about them, when to expect your next update, and how things are going.
Managing the Stress
As I’m going to talk about during tonight’s show, while IVF is not supposed to make you less stressed, it can actually make you more stressed. If there are tools out there to help you feel less stressed and less alone, I want you to definitely take advantage of those.

The other thing is one important thing that I tell my patients and their partners.
One way to communicate with a partner who is going through this, you’re standing there and you’re trying to support them, almost like a waiter, just say, “What can I do for you? How can I help you?” Just repeat, “What can I do for you? How can I help you? Is there anything that you need?”
Just knowing that there is someone out there that’s looking out for you is really helpful and makes you feel good about what you’re going through.
Join Dr. Aimee for The IVF ClassWhat IVF does NOT do
Let’s talk about some of the things that IVF does not do for you. I think a lot of people, if you look at this list, may actually think that IVF does do this.
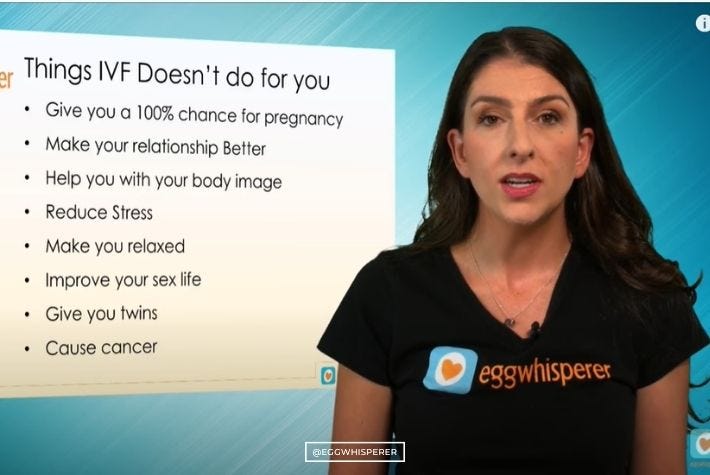
IVF Does Not Give You a 100% Chance for Pregnancy
One of the things I hear a lot is patients saying to me, “Well, I’m going to try all of this other stuff first, and then I’m going to do IVF when all of those things don’t work.” There’s almost this assumption that IVF is what you do when everything else doesn’t work because when you do IVF you’re going to have a 100% chance for pregnancy. That’s just not true. The chance for pregnancy is related to a lot of what’s going on with your genetics and the age that you’re at with the egg that you have.
For example, I’m 41, and my chance for pregnancy is 10%. When I was 31, my chance for pregnancy was probably closer to 80–85% with IVF. Knowing that going into it, you have a really good perspective going into your cycles so you know what the expectations should be so that there’s less disappointment. Then you have a better opportunity to plan how many cycles should you do, how many cycles should you expect, should you expect a good embryo the first time, do you need to do more cycles.
IVF and Pregnancy Do Not Improve Your Relationships
The other thing about IVF is maybe going into it your relationship might be a little bit rocky. I can promise you, because I’ve been around for almost 10 years now in my practice and I’ve seen a lot of stuff going on with couples, their relationships, people breaking up, getting back together, breaking up again, getting back together again. My point is that if you think that getting pregnant and having a baby is going to make your relationship better, it’s not.
What I recommend is making sure that your relationship is on solid ground before you go through treatment. You want a partner that’s supportive. You guys want to be on the same page. Talk about things like how many kids you see yourselves having, how you’re going to support yourselves through this, what you’re going to tell your family and friends as you’re going through this process. Those things are really important.
Then, as you can imagine, as you’re taking injections and you’re feeling swollen and bloated, you might not feel as good about yourself. Figure out ways so that you do feel good about yourself. These are silly things and kind of superficial, but when you’re going through something that’s making your ovaries swell and you feel like you’re walking around with big watermelons in your tummy, consider things like getting your nails done, getting your hair done, getting a massage.
Take good care of yourself and think of self-care as you’re going through something invasive like this where you’re giving yourself shots, getting lots of ultrasounds, and going through a surgery. Reward yourself with something that you like. Only you know what that’s going to be.
What about stress? For some patients, when they know they’re going into an IVF cycle, they’re actually really excited. They’re hopeful, they’re looking forward to the cycle. If you’re not one of those people, take a moment and ask yourself why. Is it maybe you don’t know what’s going on, you don’t understand the process, you don’t know what questions you should be asking, and maybe you’re not getting the information you need, you don’t know why you’re on the medications that you’re on?
Take a moment and ask your questions. I love lists. My patients send me lists all the time. They keep a nice binder with their medical records, their labs, their calendars. If you have questions about what’s going on, be sure to send those questions to your doctor ahead of time. I would say most of my patients, if not all, are very informed about the process and what they’re going through, because there’s always constant communication going back and forth. It’s important that you find a provider like that as you’re going through this procedure called IVF.
You Don’t Have to Stop Having Sex When You’re Going Through IVF
As you can imagine, when you’re getting knocked up in an IVF lab, you have your husband going to one room to do one thing while you go to another room to do another thing, it’s not that romantic. All of a sudden, people are saying now don’t have sex. What I tell my patients is you can actually still be sexual as you’re going through the process, but there are times where things shouldn’t go in certain places and things shouldn’t happen in those places. I’m just not being so explicit about what those things are, but *wink wink, nudge nudge* I think you know what I’m talking about.
IVF Does Not Increase Your Chance of Multiples
The other thing that IVF doesn’t do, and I think one of the biggest myths is that when you do IVF all of a sudden you’re going to have twins, triplets, or more. Like Octomom or Jon & Kate plus Eight, those are the kinds of terms that people throw out to me as soon as I say let’s consider IVF.

What I tell patients is your chance of having more than one baby is completely related to the number of embryos you put into someone’s uterus. If I transfer one embryo, chances are a patient will have one baby. The chance that one embryo will split into two is really low, it’s about 1%. Certainly, if I take care of hundreds and hundreds of people each year, then I will have one case of what we call monozygotic twins, but that chance is very low.
My approach to transferring is I transfer the number of embryos that I feel is going to give a patient the highest chance for having one baby at a time, and that seems to be what most doctors do. I do occasionally have patients (you know who you are) who come to me and say, “I actually really want twins,” so we have a very long discussion about the risks associated with twins.
I’m very happy to say that most of my patients with twins do well, but there certainly have been cases where patients have delivered preterm. You want to talk with your doctor about those risks. You don’t want to find out about the risks of twins after you’ve transferred two embryos. You don’t want to realize that transferring two meant twins afterward and be surprised by this.
IVF Does Not Cause Cancer
The other thing that a lot of people are fearful of, aside from the needles associated with IVF, is that IVF causes long-term issues with your health, especially if you’ve done multiple cycles. A question I get often is, “How many cycles can I safely do?” We know from studies that IVF actually does not cause breast cancer and it does not cause ovarian cancer.
When I talk to a patient, I talk to them about their individual genetics and family history, what they know about themselves. Do they know if their family history is significant for things like breast cancer or ovarian cancer? If someone has a genetic predisposition for a cancer like that, I’m going to offer them a genetic cancer screen. It doesn’t mean that you can’t go through treatment, but there definitely is a different approach that we take so that patients aren’t exposed to as much estrogen compared to other protocols that we may use.
What IVF Does
I talked to you a little bit about what IVF doesn’t do, and I sound really negative about IVF, but I think that IVF is one of the greatest inventions ever. It was invented to help young women get pregnant who have blocked fallopian tubes. Here we are now and there are so many other reasons why we use it. Not just blocked fallopian tubes, but low sperm counts, and we use it in older women. It is a great invention, as far as I’m concerned.

IVF Preserves Your Embryos for The Future
Some of the other options that people use IVF for is to preserve embryos for their future. One of the conversations that I have with my patients is about fertility preservation. I always ask my patients, “How many kids do you want?” I totally get it when you’ve been struggling for years, you look at me like, “Seriously? I just want one baby, after everything we’ve been through.”
But when you’re considering IVF, there are times, a lot of times, where a patient can actually perhaps do more than one cycle because she wants three or four children. I have had patients come to me and say, “I want a big family. I want a family of three or four.” We just take our time and we do the number of cycles that we need to make sure that she has enough embryos that are strong enough to give her that size family that she wants.
That’s what fertility preservation means. It doesn’t just refer to freezing eggs or freezing sperm, but you can actually freeze embryos to use in the future. Unlike the bagel that’s sitting in my freezer right now that has lots of freezer burn and I’ll probably never eat it, embryos aren’t like that. As long as human beings are around, you can thaw them indefinitely. Human beings that know how to thaw embryos, of course.
IVF Allows You To Genetically Test Embryos
Another good thing about IVF is that you can genetically test embryos. As soon as some people hear that, what they start thinking is this word ‘designer babies.’ You can’t turn an embryo into a male or a female embryo. You can’t turn an embryo into a blue-eyed, blonde-haired baby, or a tall baby, or a baby that will play basketball or swim like Michael Phelps. That’s just not possible. All we can do when we genetically test embryos is find out if an embryo has a balanced number of chromosomes. If an embryo has an extra chromosome or is missing a chromosome, that embryo may not be compatible with a healthy pregnancy.
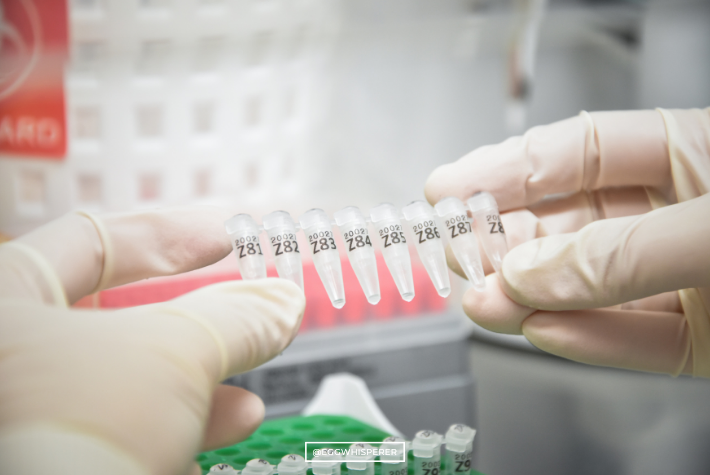
Those are some of the things that you may choose to do. In my practice, I offer genetic testing to everyone. I want everyone to understand the technology and see if it’s right for them, and also speak with a geneticist about the technology and the drawbacks. It’s not perfect. I call PGS, which stands for preimplantation genetic screening, the murky crystal ball in IVF medicine. It certainly isn’t perfect, but for now it’s the best that we have.
If it’s something that you’re going to choose to do, talk to your doctor about it, talk to them about the pitfalls, talk to them about why they think it might be something for you to consider. The other thing that you should know, if you don’t do it upfront, and let’s say you freeze your embryos, and you have many embryos after your successful transfer, you can certainly go back and test your embryos later.
There’s a term you may hear, family balancing. Some people consider it controversial, but I feel like if you’ve gone through all of this and you want to know the gender of your embryos, it’s really up to you to know. For your next pregnancy, let’s say you have the opportunity to look at the gender because your doctor offers that to you, you can then say, “I have a boy. Next time I’ll have a girl.” But we can’t turn an embryo into a male embryo or a girl embryo.
IVF Gives the Highest Pregnancy Rate of Fertility Treatments
The other great thing about IVF is that it gives us the highest pregnancy rate compared to any fertility treatment that’s out there. Let’s just say for example, natural conception rates for a 30-year-old per cycle, it’s about 15%. IUI pregnancy rates might be 12–15%, depending on what study you read. IVF really takes you all the way up there much higher, over 65%. The reason is that IVF bypasses the embryo transport system, and that embryo transport system is the fallopian tube.
I’m just going to do this right now (Imagine Dr. Aimee acting like a uterus with arms acting like tubes). Pretend that this egg is sitting right here in the fallopian tube (Dr. Aimees’ arm). That’s a funky tube, but this tube is open. The sperm is now going right here, and they’re meeting here. We have to rely on lots of stuff to go right in order for the embryo to land in the uterus. But when you’re doing IVF, the embryo is just landing in the uterus. That’s why the pregnancy rates are much higher with IVF than they are at home.
Trust me, it’s still not dangerous to get pregnant at home. It’s way more romantic. My approach with my patients is I want to learn everything there is to learn about you, figure out what your diagnosis is, so that if I’m giving you the highest pregnancy rate at home, meaning I’ve optimized everything with exercise, supplements, lifestyle tips, then when it comes to doing IVF, you’ll hopefully have the highest chance possible.
Some of the Cons of IVF
Let’s talk about some of the cons. Some of the things that you might want to go into your IVF cycle knowing so that, not necessarily these things don’t happen to you, but if they do, you’ll know what to do in case that happens.

IVF Can Be Emotionally Draining
What I find is the hardest part of IVF, certainly it’s involved, but the emotional cost is so great, especially if the cycle doesn’t work. It’s kind of like if it’s raining, you bring an umbrella. It’s nice to have an umbrella just in case next time you go outside, if it rains, you have it. Just talking through with your partner or with a fertility therapist, or talk to yourself in the shower, about what am I going to do if this cycle doesn’t work.

Talk through that before the cycle starts so that you have an idea as to what are we going to do. Because at the end of the day we’re talking about an egg, and that’s a human egg, with a sperm cell, and that just means a chance for pregnancy. Not every cycle results in a successful transfer. Knowing what your chances are and knowing what the emotional cost might be if something doesn’t work, it’s important to talk through that and what you’re going to do and how you’re going to be supported by your family and friends. Knowing that upfront can make the experience so much better for you.
IVF Can Be Expensive
Then there’s the financial cost. Making sure that you know what things cost, how much money you should have set aside, and then talking to the financial counselor at your clinic to get a really good idea about that part of things and if they have any plans or financing programs available to you.
IVF Impacts Your Body
The other few things that can also happen during a cycle is pain. Going through IVF means having a surgery. I wish that there was a way that a woman can just take her eggs and put it in a cup (egg ejaculation ha! not so fast), but we can’t do that.
Back to my tips on the other things that can happen with your IVF cycle, and that’s the pain.
After the egg retrieval, you’ll feel really crampy. I have patients when they get their IVF medications they’re always like, “Aimee, why did you give me Tylenol#3?” I say I just want you to have it. 95% of my patients don’t need it, but the 5% that do are really happy that they have it. After the egg retrieval, your ovaries get swollen and it’s harder to walk, it’s harder to move, and it’s harder to sleep, especially that first night. With just a little bit of pain medication, it’s going to be fine.
I think a lot of patients are fearful of taking pain medication because they somehow think it’s going to interfere with their future pregnancy, that somehow taking pain medication might make the likelihood of success lower. But, in fact, it doesn’t. These medications are just in your system for about six to eight hours.
Pain is one of those things that is totally treatable. If you have severe pain, it’s really important to talk to your doctor right away, because there are three serious complications that can come from IVF. One is a twisted ovary, that can happen around 1% or less of the time. A ruptured ovarian cyst, also 1% or less of the time and lastly, OHSS.
OHSS
OHSS, causes severe swelling and bloating in your tummy and fluid build-up as well. There are ways to deal with that, and one way is to be seen very often. My patients will see me on average five times during their IVF cycle. As I’m watching their ovaries grow, I’m titrating their medications, I’m giving recommendations for when they should slow down on their exercise, when they should stop exercise completely, when they should start drinking electrolyte rich and protein rich drinks, about one liter per day.
This is really for women who have on average 15 follicles or more. Women who have an estradiol level over about 2,000 or 2,300, approximately, are the ones who are at greatest risk for having OHSS. By doing a combination of a Lupron trigger with a low dose HCG or just Lupron alone, there are other drugs as well that can lower prolactin levels, lower estrogen levels, that can also be used to protect patients from having serious complications from IVF.
Know All of Your Options
I have patients that say to me, “Aimee, I don’t want to do IVF because I don’t want to have embryos frozen.” Then I can say you don’t have to have embryos frozen. We can collect (I’ll just throw out a number) 10 eggs, and then we can fertilize maybe two of them, and freeze the rest as eggs. You definitely can work with your doctor, talk to them about your feelings about the process and what you feel is right for you.

Know all of the options going forward. The last thing I would want is someone to go through the process and have lots of embryos frozen and then feel really sad that they’re not going to be able to use those embryos in the future. Obviously, there are things like embryo donation, which are great ways to help other families, but that may not be right for you. Talk to your doctor about whether you should freeze some eggs first so you have a plan for unused embryos before they are created.


