Get Organized — the old fashioned-way
- Paper
- Pen
- Three Ring Binder with Dividers: Include your medical records, your labs, your medication calendar, and receipts so you can keep everything in one place.
Understand what your IVF pyramid looks like
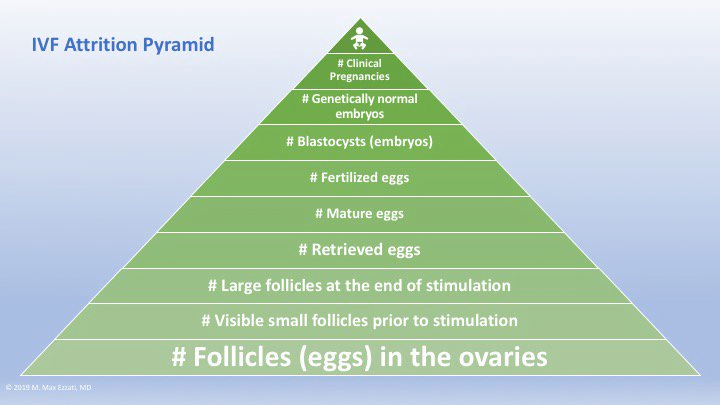
So often in IVF, we talk about things in terms of depletion. What are you losing? For example, you start off with a certain number of eggs at the beginning of the cycle. That’s called the antral follicle count. As the cycle progresses sometimes not all of those eggs grow. In the end, for example, you may gain two healthy embryos from ten follicles and so it is a natural and normal human response to feel like something is lost and that something was taken away from you. I want to flip that on its head.
Instead, you’ve started with ten eggs from which you’ve now gained two embryos. So it took ten follicles to get the two eggs from that cycle.
Here’s another example:
So let’s say you have ten follicles, and of those follicles you have nine eggs retrieved. Out of the nine retrieved, let’s say eight are mature. Of the eight, six were fertilized and three blastocysts form from that six. Of those three, two are normal and now we go on and have one baby.
That is the IVF pyramid. This pyramid is customized to you. Your pyramid is built according to your age, your follicle count, your AMH level, and what your doctor knows about you. I think it’s important to know these numbers upfront because numbers in IVF don’t work like numbers do in just about everything else in our life. What do I mean? 10 eggs don’t necessarily mean 10 healthy embryos. You need to have the right set of expectations going into it. If you have 10 eggs and you get 2 embryos and your doctor is super happy, but you’re upset, then the right expectations were not set.
I like people to feel like they are informed.
Ask your doctor a simple question:
How many healthy embryos do you expect from the number of follicles that I have?
Your doctor should be able to give you a good indication based on your age, AMH level, FSH level. What do they think?
How many healthy embryos do you think I’ll get from this cycle?
Questions to ask yourself
What is your diagnosis?
Why am I doing this?
I always recommend getting your TUSHY checked.
What can I do that’s in my power to give myself the highest chance for pregnancy?
To get the answer from a doctor that your fertility is unexplained is NOT an answer. So many patients come to me with that diagnosis.
There is always an explanation. Find a doctor that will tell you what the answer is. Ask your doctor “What are the possible explanations in my case?” Sperm quality issues may be at the heart of the problem. Don’t sugar coat them. Talk about them before your cycle so you can do everything in your control to improve them.
Along the lines of the IVF pyramid. Continue to ask your doctor questions like:
What are my chances?
How many cycles will it take?
Get answers to these questions before your IVF cycles start. It will put you at ease. Asking these questions helps you to get better informed. I want you to know as much as you can about your own IVF cycle. Do your homework!
Questions to Ask Your Doctor
It’s okay to ask questions!
What protocol are we using and why?
What medications am I using and why?
What side effects can I expect?
If you didn’t know, for example, that you were going to feel bloated then it might be very upsetting and worry you when this is likely to happen.
I tell my patients that at the beginning they may feel nauseous, experience breast tenderness, and might even feel some twinges in their ovaries. As the cycle progresses you might see some cervical mucus and that’s totally normal. That’s your body’s natural response to rising estrogen levels.
Someone told me today she felt like a whale or an elephant walking around. If that is a symptom that you don’t want to feel and something you deem not worth going through IVF for then you need to know that up front. There are ways to adjust things so the approach is gentler and the symptoms milder. I promise you it is not easy to be an IVF patient. However, if you go into it with the right expectations then you might think, “yeah — I knew this was going to happen. I can totally handle it.”
When should I stop exercising and stop having sex?
I tell my patients that they don’t need to abstain from sex. You’re on all of these hormones and may want to have sex. It would be cruel for me to tell you that you can’t do it. However, you may also feel bloated and not thrilled about the idea of sex. To which I tell you to consider outercourse. If you don’t know what that is, google it!
As far as exercising goes, listen to your body. If you feel like running, then run. Certainly, there comes a point where you shouldn’t run. I ask my patients to stop running after three days of treatment. If your body is cramping then slow it down. Do some walking, yoga, or pilates. After the transfer, please take it slow. Now is not the time for high-intensity fitness. Talk to your doctor. They know you best.
What foods should I eat?
This is individualized. Don’t force yourself to eat something if you know you won’t like it. You’ll often hear me talk about the Mediterranean diet or the pro fertility diet. The pro fertility diet consists of low pesticide produce, fish, whole grains, and dairy. Chances are many of you already do this. Fresh fruits and vegetables — these are the types of things that you want to focus on. Avoid plastics too.
What supplements should I take?
I believe that supplements help. I ask my patients to take a good prenatal vitamin, Vitamin D supplement, coQ10, and fish oil. I also individualize this list. There are other patients that I ask to take other things like, for example, acai berry, melatonin, or DHEA. There’s certainly no one-size-fits-all approach to supplements so please talk to your doctor first.
Are you ready for more?
Good, because I have MORE recommendations.
You may be thinking, “Geesh — does she get tired of telling her patients all of this?” The answer is an emphatic, no!
I put everything I have into helping my patients. I do all the ultrasounds and procedures myself. If something doesn’t work then it feels like my loss as well. I want my patients to be wildly successful.
Therapist & Acupuncturist:
Consider adding these professionals to your Fertility T.E.A.M. An acupuncturist can certainly help with the symptoms you’re likely to experience through the cycle. Therapy can help deal with all of the relationship stress or the personal emotional experience of going through IVF. They will equip you with all sorts of techniques. Things like, “find your happy place.” But there are so many other techniques you can use to reduce stress. They will also help you talk through your feelings about possibly having unused embryos. It’s very important to talk about this before IVF. Depending on how you feel, you may want the option of freezing eggs instead of fertilizing all the eggs retrieved.

When I have patients that are extremely needle phobic I have them come to my office and I mix the shots for them and administer them myself. However, if you don’t want to do that, that’s okay there’s this thing called the buzzy bee. It is an ice pack that vibrates when placed on your skin. The ice numbing your skin and the vibration work together to lessen the chance that you’ll feel the needle. If this is something that interests you it can be found online.
This is another option similar to the buzzy bee. It’s basically a sticky ice pack that you apply to your skin prior to administering a shot.
As you go through the process you’re going to feel crampy. This is especially true after the retrieval. A heating pad may become your best friend to help make you feel comfortable. This is true even when you have a period at the start of IVF. Tylenol, Motrin, the heating pad — these may all help.
Stool softener:
As your ovaries get swollen, guess what also happens? Your bowels may slow. This may also happen due to a reaction to the anesthesia medications. We don’t want a poop emergency. You don’t want to go to the E.R. because you’re super constipated. Taking a stool softener like Colace can really help during this process. This is one of the things I tell my patients to prepare and have on-hand before going through IVF. I want you to avoid having to go to the pharmacy mid-poop emergency and be pondering all of your stool softener options. There are many! Pick one up in advance. You may use it during IVF, pregnancy or even postpartum.
Electrolyte-rich drinks:
I call it salty water. Coconut water, G2, Powerade, and many more drinks are available that can help you stay hydrated.
IVF Egg Whisperer Pants:
These are new pants I have designed that will be available soon. My goal with these pants is to enable a more comfortable fertility visit so you’re not feeling so exposed when you wait for the doctor to come in. I want the experience to be as comfortable as possible for my patients and IVF patients everywhere. If you’re interested in these pants please email me, email@eggwhisperer.com, to be notified when they are available.
Protein bars & shakes:
My favorite brand is Orgain. They make organic protein bars and ready-made shakes. I don’t have much patience with powder to mix and make custom protein shakes. They are super tasty and healthy. When you’re feeling really bloated and not wanting to eat a full meal sometimes these can be a good back up option.
Tylenol & Motrin:
Have this at home for headaches and cramps. I recommend you always talk to your doctor about what you’re taking or plan to take so that they can confirm it is the best option for you.
Electrolyte powders:
Liquid IV or Drip Drop are options to add the powder to water to make it more hydrating.
Anti-itch Cream:
It is not unusual to get a reaction to some of the shots. You can get a raised red reaction when you take the trigger shot. So when a patient messages me that they have this I just tell them to put on the anti-itch cream.
Benadryl:
Consider taking at night if you experience itchiness from the progesterone shots.
Claritin:
Consider taking this before you administer shots if you know you’re prone to itchiness.
Again, please talk to your doctor about any medication before you take it!
No, not a vibrator, but a massage stick! Like a hand roller massager where you can put over the shot where you put the progesterone. If you think this would be helpful for you before your shots, then go find one.
Self Care:
This is super important. We are all stressed. Everyone is anxious. We are dealing with so many things. We are trying to maintain relationships with work, friends, family, our partner if we have one.
This is what I tell my patients. We are so much better together than alone. I want you to find someone you can depend on. Not just a person online in a group chat forum, but I am talking about a true friend. Someone that can come to appointments and be on call for you.
Shine Fertility or Fruitful Fertility are two sites that match up with patients those that have gone through a similar fertility journeys. These are mentorship programs and can be very helpful.
You can also talk to your doctor. I have matched up patients who are going through the same thing so they can support one another.
I have previous patients that have volunteered to be mentors to patients and it’s been a very positive experience.
I highly recommend you do not go through this alone. Fertility warriors are people that want to connect with others so they don’t feel alone as they may have. Trust me, we are better together!
Here’s my self-care checklist:
- Take one nature walk each week. It just changes your mood to be in nature. Pick out one place each week to do it. Go alone, with a friend, or a partner.
- Decide on one thing you will do to pamper yourself each week. This doesn’t have to be each week, it can be every other week or twice a week! It can be something to relax you — a massage, a pedicure. Whatever it is, make it for you.
- Decide who you will share your journey with, and when. Talk to your partner about this too. You don’t want any surprises with what your partner has shared. Be on the same page. If you tell people you’re going through IVF they will remember. I want you to think about this before you go through your IVF cycle. They can watch this show or read this blog to learn how to be the best support partner to you in IVF.
How to Prepare for Transfer:
Now we’re preparing for transfer and here’s your checklist. Ask these questions or yourself and to your doctor.
Are you going to do a fresh or frozen transfer?
If you don’t know the difference between these two it is imperative that you know before you go through your transfer. A fresh transfer is transferring about 5 days after the egg retrieval. That’s typically what I do. I transfer embryos that reach the stage called the blastocyst stage — they have hundreds of cells. These are the embryos that are the most viable and give patients the highest chance of pregnancy.
Will you be conducting genetic testing on the embryos?
I also talk to my patients about genetic testing so they can find out which embryo has a normal set of chromosomes before transferring. It seems that might give patients a higher chance of pregnancy and a lower risk of miscarriage and you can also preserve your fertility and find out which embryos to use next time, for your next pregnancy. Hopefully, that means another pregnancy and not another transfer if the first transfer didn’t work.
How will you prepare for that transfer?
You have to meet with someone and talk with them and have them walk through with you what preparation means based on what they know about you.
What are the steps you’re going to take? Have you done a mock transfer? Are you going to do implantation testing? Have you done a saline sonogram to look to see if you have, for example, a uterine polyp?
Preparation is so important.
If you’re considering a fresh transfer then I want you to know these things before the embryos come in. I see patients from all over the world. I do video consults with them and when I ask, “What was your embryo quality at the time of your transfer?”
I’m surprised that many people tell me they don’t know. Either they don’t know there was a grade of embryo quality, they didn’t know they could ask, or they simply were not told that information.
I’m hopeful that will change. I want all of you to know that embryos are like diamonds in that they are assigned scores. That score is related to implantation potential and knowing this number helps inform how many more cycles it might take for us to be successful.
Know the quality of your embryos at the time of transfer. It’s super important!
How many embryos should I transfer to give me the highest chance of a healthy pregnancy?
A lot of times it means one. For patients over a certain age, it means up to four transfers. Talk to your doctor about this beforehand, even on your transfer day!
The other thing to consider if you don’t already have kids at home and want to consider having more is the idea of banking embryos. This is for people that don’t have other frozen embryos for the future but may want more than one child.
Do I have a hydrosalpinx (a fallopian tube that’s blocked with a watery fluid)?
Am I at risk for an ectopic pregnancy?
Should I do a hysteroscopy for a polyp first?
Do I have endometriosis that needs to be treated before a transfer?
Going through this checklist here will make sure you don’t need to do anything more before moving forward with your IVF cycle.
Let it Go:
Once you’ve done or considered everything on this list (and maybe more!) then I tell my patients to just, “Let it go.”
You’ve done all the homework and everything you possibly can. The only thing you can do is to trust the process.
In Conclusion:
I hope this was helpful. I love talking about fertility.
If you’re going through IVF right now and there’s something I haven’t mentioned that you have found helpful to you, I want to hear about it! Please mention it in the comments or send me a note at email@eggwhisperer.com.
I’d love to hear from you so that we can create the most comprehensive IVF recommendation checklist of all time. I won’t be here forever, but maybe this list can!
You can also catch more of me and topics like this through The Egg Whisperer Show. The episodes are live-streamed onYouTube,Facebook, and Twitter and on Wednesdays at 7 PM PST. Subscribe to the podcast too!

